These recommendations are based on observational evidence, and due to the limited data, there is no consensus on the need of follow-ups after the initial screening. While the current guidelines suggest the use of transthoracic echocardiography to rule out structural heart disease in isolated LBBB, the recommendation is less stringent in patients with conduction disorders other than LBBB (Kusumoto et al., 2018). Only two prior population studies have assessed the clinical significance of incomplete LBBB (iLBBB) and found no relation to CV mortality (Haataja et al., 2015) (Tervahauta, Pekkanen, Punsar, & Nissinen, 1996). Somewhat surprisingly, one previous study found that incomplete RBBB (iRBBB) was associated with increased all-cause and CV mortality (Haataja et al., 2015).
LBBB VS IVCD FREE
Previous scientific literature does not provide much information about the prevalence or prognostic significance of incomplete bundle branch blocks in individuals apparently free of CV disease. Isolated left posterior fascicular block (LPFB) is a rare conduction disorder with no clear consensus on prognostic significance without CV disease (Pérez-Riera et al., 2018). Left anterior fascicular block (LAFB) is usually regarded as a conduction disorder without clinical significance if encountered in asymptomatic individuals (Elizari, Acunzo, and Ferreiro, 2007). The effect of the ECG definitions of LBBB and NSIVCD on outcome has not been reported in prior population studies. On the other hand, non-specific IVCD (NSIVCD) is considered as an ECG marker of adverse outcome due to its potential association with structural heart disease (Eschalier et al., 2015 Haataja et al., 2015). The results of studies evaluating the prognostic impact of LBBB on all-cause mortality in subjects without known CV disease are also somewhat conflicting (Haataja et al., 2015 Imanishi et al., 2006 Schneider, Thomas, Kreger, McNamara, & Kannel, 1979), and even the standard electrocardiographic (ECG) criteria for LBBB have been challenged (Strauss, Selvester, & Wagner, 2011). Some authors showed that RBBB was associated with increased all-cause mortality, while other investigators found no effect on outcome (Bussink et al., 2013 Haataja et al., 2015).
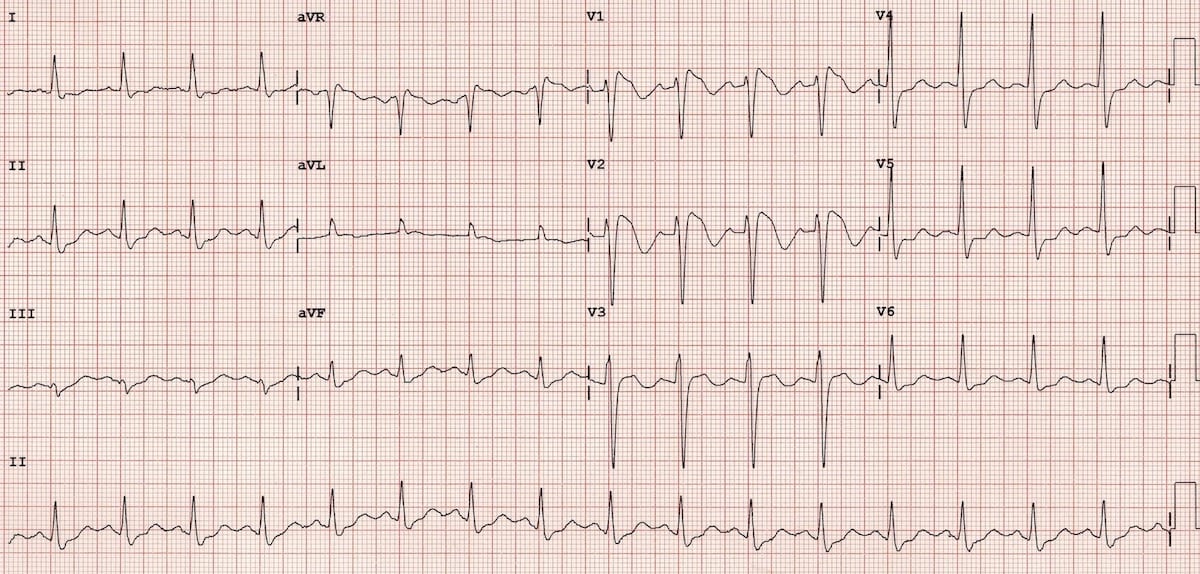
In subjects with IVCDs without other evidence of cardiac disease (isolated bundle branch block), published reports show conflicting results. Both right (RBBB) and left bundle branch blocks (LBBB) are associated with adverse outcome in subjects with overt cardiovascular disease (CV Wang et al., 2008 Zhang et al., 2012). The clinical significance of various intraventricular conduction delays (IVCD) depends on the type of the conduction disorder and on the studied patient population. The prognostic impact of LBBB and NSIVCD was affected by the definition of the conduction disorder.
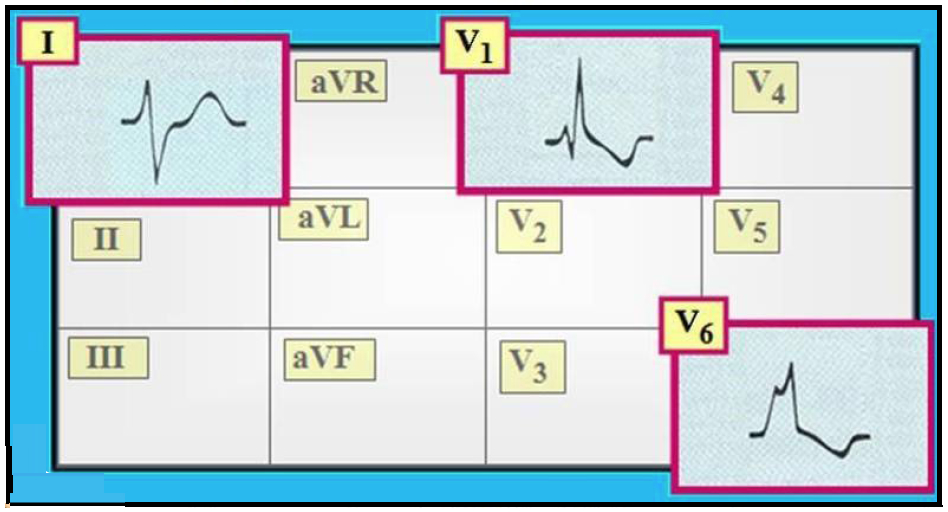
Other IVCDs had no significant impact on prognosis. In a population study with long-term follow-up, NSIVCD and Minnesota definition of LBBB were independently associated with CV mortality.
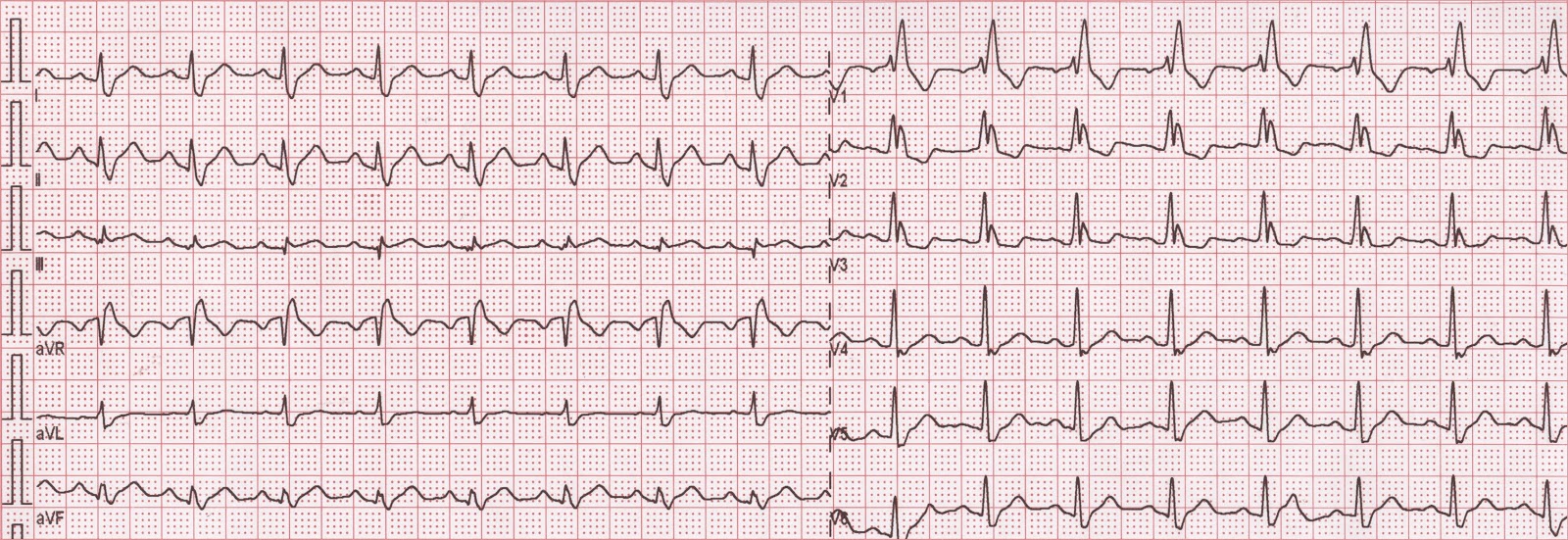
The presence of R-R’ pattern was not associated with any adverse outcome. While right bundle branch block, left anterior fascicular block and incomplete bundle branch blocks were associated with seemingly higher mortality, this was no longer the case after adjustment for age and sex. Subjects with NSIVCD were associated with twofold to threefold increase in CV mortality depending on the definition. After controlling for known clinical risk factors, the hazard ratio for CV death, compared with individuals without IVCD, was 1.55 for the Minnesota definition of LBBB (95% confidence interval 1.04–2.31, p = .032) and 1.27 (95% confidence interval 0.80–2.02, p = .308) for the Strauss’ definition of LBBB. Resultsĭuring 16.5 years’ follow-up, 1,309 of the 6,299 subjects (20.8%) died and of these 655 (10.4%) were cardiovascular (CV) deaths. For left bundle branch block (LBBB) and non-specific IVCD (NSIVCD), two different definitions were used. We studied long-term prognostic impact and the association with comorbidities of eight IVCDs in a random sample of 6,299 Finnish subjects (2,857 men and 3,442 women, mean age 52.8, SD 14.9 years) aged 30 or over who participated in the health examination including 12-lead ECG. Previous population studies have presented conflicting results regarding the prognostic impact of intraventricular conduction delays (IVCD).
